During World Breastfeeding Week #WBW2019, we are hosting a series of guest blogs exploring how the wider team of health professionals and community breastfeeding support can support breastfeeding families. The WBTi Report found numerous gaps in health professional training in infant feeding, and we are delighted to see a terrific range of resources being developed to address this.
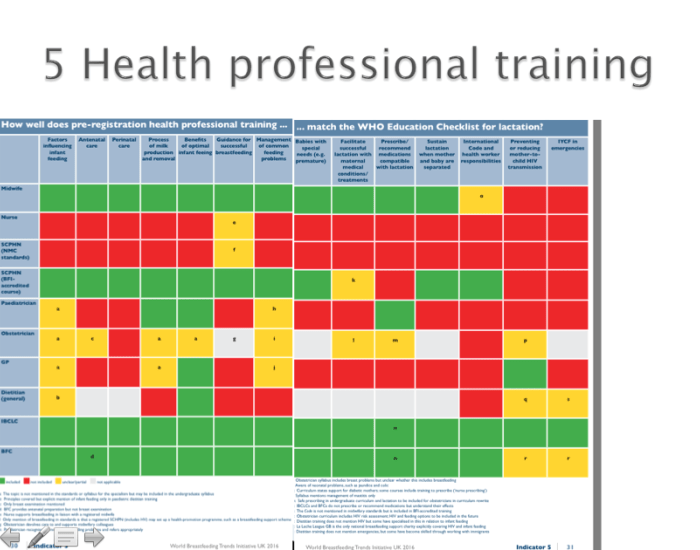
For details of gaps in health professional training, see “Indicator 5” in Part 1 of the WBTi Report for the summary table above and in Part 2 for the detailed findings on each health profession.
There is exciting progress to strengthen breastfeeding education and policy in a hospital setting in the UK, with the launch of a comprehensive website resource for hospital health professionals this week www.hifn.org. Co-chair Ilana Levene tells us more about the Hospital Infant Feeding Network (HIFN).
“HIFN was set up in 2018 and consists of a network of health professionals interested in supporting and facilitating breastfeeding in a hospital setting in the United Kingdom. I’m a paediatric trainee with a special interest in neonatal nutrition and my co-chair Vicky Thomas is a consultant paediatrician with a special interest in complex nutritional difficulties in infancy and childhood. Our steering committee includes a parent, a nurse practitioner, a dietitian and doctors from other specialities such as anaesthetics, endocrinology and emergency medicine. All health professionals and those who have a strong interest in hospital breastfeeding are welcome to become active within HIFN – if you would like to join, please search for the closed Facebook Group “Hospital Infant Feeding Network” and follow us on Twitter @HIFN12. To understand more about HIFN, just dive right into our new website www.hifn.org, launching this week to mark World Breastfeeding Week. It covers our principles and goals, general background issues of infant feeding in the UK and specific topics relevant to health professionals looking after both mothers and children in a hospital setting. If you’re not a hospital health professional, signpost those you know to the website as a source of expert, referenced, practical breastfeeding-friendly knowledge.
Why did we decide to form a new network for hospital health professionals? In 2016, the GP Infant Feeding Network (GPIFN) was set up in order to improve infant feeding support by General Practitioners, and this arena showed that there was a significant appetite and unmet need not only from GPs, but also hospital professionals. A recent survey of paediatric doctors in a large UK hospital found that 30% did not agree that breastfeeding is the most beneficial form of nutrition in the first 6 months of life, and over 50% felt inadequately trained to manage breastfeeding when they encounter it. WBTi has documented the many gaps in undergraduate and postgraduate training (see Indicator 5 in both Part 1 and Pat 2 of the WBTi report) , and sources like the parent-led Hospital Breastfeeding campaign have clearly shown the poor practice families experience on the ground every day as a result. With this pressing need in mind, a group of hospital professionals active in GPIFN decided to form a sister network. From the moment of inception, we have reached out to families, the lay organisations active in the breastfeeding field, and lactation professionals, in order to work in partnership.
Apart from working on our website content, HIFN has achieved major campaigning wins through advocacy with the Royal College of Paediatrics and Child Health, who recently announced they will no longer accept any funding from breastmilk substitute manufacturers. This has started to ripple out to other associated organisations such as the British Association of Perinatal Medicine. We re-launched a longstanding campaign related to medication in lactation, alongside GPIFN and the Breastfeeding Network, and with support from the UK Drugs in Lactation Advisory Service, called #dontsaystoplookitup. We provided poster resources for National Breastfeeding Celebration weeks – both of these sets of resources are available for download on the website www.hifn.org/dontsaystop and www.hifn.org/posters.
We look forward to continuing to serve UK families moving forward and welcome you to have a look at the new website and get more health professionals involved.”

Ilana Levene is a paediatric doctor planning to sub-specialise in neonatal medicine and interested in research relating to neonatal nutrition. She lives in Oxford with her husband, an environmental consultant, and two children. She is a trustee of Oxfordshire Breastfeeding Support, a local grassroots network of free weekly breastfeeding drop-ins and online support. She likes cross-stitching and making patchwork quilts.