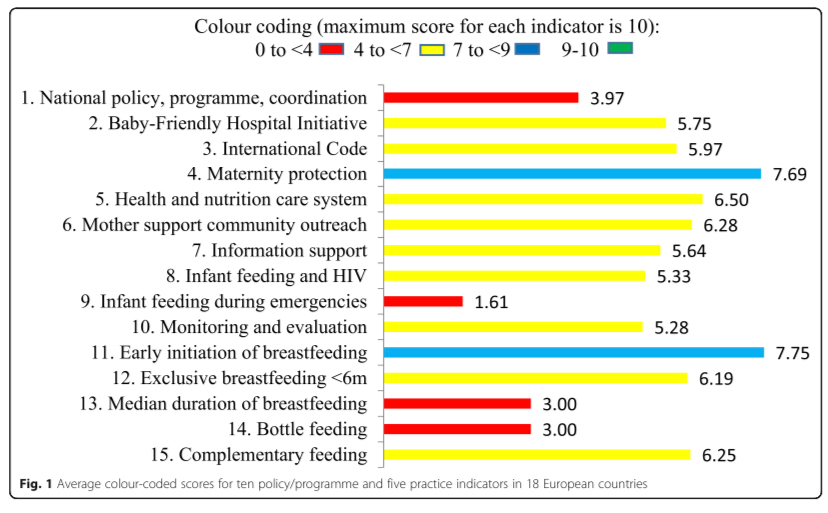
Our WBTi work has revealed that in the UK we have no national guidance on the support and feeding of infants and young children, or pregnant or breastfeeding mothers, during emergencies. There is currently a postcode lottery of Local Resilience Forums who include a few details in their advice to the public such as “Remember to pack formula and nappies for your baby”, but there is no national guidance for LRFs and local authorities that they should include infants and young children in their planning.
This page will serve as a repository for resources for those planning services and those providing feeding support for Ukrainian families with infants and young children.
Breastfeeding provides infants with food security, immune protection, and emotional comfort during disasters.
Basic priorities in an emergency:1) Support new mothers to hold their babies skin to skin and begin breastfeeding within the first hour.
2) Support mothers who are breastfeeding, partially or fully breastfeeding, to continue breastfeeding and increase their milk supply if needed: provide access to skilled feeding support.
3) Protect infants who are not breastfed: Trained infant feeding / nutrition support teams from trusted NGOs like UNICEF will provide access to safe supplies of appropriate infant formula for babies that need it, and support with safe preparation under hazardous conditions.
4) Protect all infants: breastmilk substitutes and feeding equipment (infant formulas and other milks, bottles, teats, breast pumps and also donor human milk) will be provided by trusted NGOs like UNICEF; the public should AVOID sending donations of these into high risk settings, but send donations of funds to trusted NGOS instead. This will enable them to provide families with what is needed on the ground.

We have collected links to infant feeding resources in Ukrainian, and also in the languages of countries housing refugee families, for breastfeeding helpers and aid workers in those countries.
Please send us any suggestions for additional resources
We have a few other resources not included here; please email us any enquiries.
NOTE: we will continue to add links and resources to this page, and these organisations are continuing to add further translations into more languages – please make sure that you clear your cache, or ‘refresh’ the page, each time you open any of these links to ensure that you find the most up to date page.
NOTE: We are providing these resources as a public service, but we cannot read the resources in other languages ourselves, so we cannot always vouch for the accuracy of the contents. Please have someone fluent in the language read it for you.
CONTACT: wbti@ukbreastfeeding.org
WHERE TO START? Watch this 4 minute introductory video from Save the Children
Aid worker or emergency planner? Short video here: how can you incorporate best practice into your support for Ukrainian families?
GET INFORMED: Read the first 25 pages of the Guidance for an overview of best practice.
Resources from the Global Breastfeeding Collective, led by WHO and UNICEF
It is important to continue breastfeeding if you are COVID positive: your milk can pass antibodies to your baby! More resources HERE.
UNICEF UK Baby Friendly resources
Guidance for local authorities on infant feeding during COVID19 (from BFI, First Steps Nutrition Trust, and NIFN). First line guidance for UK local authorities responsible for supporting families
The provision of formula in food banks (November 2020)
Statement on infant formula in food banks (November 2020) – signposting
See also the response to Question 11 on formula donations and distribution in their FAQ here
International humanitarian guidelines and operational guidance
Operational Guidance on Infant feeding in Emergencies
for Emergency Relief Staff and Programme Managers
Available in numerous languages
Media Guide and Guide on writing/ talking about infant feeding in emergencies
These are extremely useful for humanitarian aid organisations and for the media in framing the situation
Guidance for helpers not trained in supporting infant feeding
This short leaflet was written for local authorities and those supporting Afghan refugee families but could be useful for those supporting Ukrainian refugees in the UK. It sets the context, lists some useful resources for parents, provides information about making up powdered infant formula correctly and describes useful actions in some possible scenarios.
Infant feeding support resources – multiple languages
Rapid Feeding Assessment Key Phrases in multiple languages (including Ukrainian, Russian, Romanian, Polish and English – scroll down the page)
Simple Points for Helpers – infant feeding in emergencies in multiple languages (including Ukrainian, Russian, Romanian, Polish and English – scroll down the page)
Pictorial counselling cards in many languages including Russian, adapted to include COVID19 recommendations. Some are full pictorial sets, while some are simply the translation matrix.
Infant Feeding flyer for families in transit (including English, Ukrainian, Polish, Russian, updated for COVID19). Developed by the volunteer team from Infant Feeding Support for Refugee Children/ Safely Fed
Posters and booklets in Ukrainian hosted by the Lithuanian IBCLC Association
Pictorial book about breastfeeding (no words) from La Leche League Netherlands. The PDF is free to use for all. Printing and sharing is allowed, as long as the original file (including credits) is unaltered. Price listed on website is for printed version.
Breastfeeding resources in multiple languages including Ukrainian, Romanian, Russian. (From the Missouri Department of Health and Senior Services, USA)
Breastfeeding Matters – A Guide to Breastfeeding for Women and their Families (from best Start, Ontario Canada) can be downloaded free in Russian and other languages
Translations of key phrases, breastfeeding infographics in many languages, and more: Safely Fed European resources
La Leche League International: Variety of resources and infographics in infant feeding in emergencies translated into multiple languages – most are directed at mothers and parents
Global Health Media: Videos on childbirth and breastfeeding topics.
Infant Feeding in Emergencies Social Media resources:
Infant Feeding Support for Refugee Children Facebook Page: Memes/ graphics in multiple languages, with appropriate captions
La Leche League International Facebook page: Memes/ graphics in multiple languages, aimed at mothers and parents
Safely Fed UK Facebook page – volunteers welcome to create graphics in Canva and to monitor the page! Contact WBTi UK: wbti@ukbreastfeeding.org
For policy makers, emergency planners, media and humanitarian aid workers
Policy resources, media guide, training materials: Infant Feeding in Emergencies Core Group
IYCFE Hub: global hub of resources
Background information on breastfeeding in Ukraine: WBTi 2015 Ukraine Assessment Report
Policy resources, translations of key phrases, and more: Safely Fed European resources
Please do contact us if you are interested in volunteering or have some useful resources to share!!
CONTACT: wbti@ukbreastfeeding.org